When a patient comes to the podiatrist with heel pain, it is common to find that this pain stems from a condition called plantar fasciitis.
While less well-known than other foot conditions like bunions or hammer toe, it is equally distressing and can have a significant impact on quality of life.
History and Anatomy of Plantar Fasciitis
Plantar fasciitis is an inflammation of the plantar fascia, a thick band of tissue that connects the heel to the toes. It runs along the arch of the foot, supporting the foot’s arch. Looking back in history, we find that while plantar fasciitis has been studied for decades, its prevalence has increased with the rise of physical activities and sedentary lifestyles.
The foot’s anatomy is complex, with its numerous bones, joints, ligaments, and tendons. A deformity or imbalance in one part of the foot can lead to pain elsewhere. For example, toe deformities, such as hammer toe, claw toe, or mallet toe, can affect how weight is distributed on the foot, thereby exacerbating plantar fasciitis.
The Importance of the Foot Arch
The foot arch, the natural curve seen on the inner side of the foot, plays a pivotal role in various foot functions. It acts as a shock absorber during walking, running, or any movement, dissipating impact forces that otherwise transmit through the body. The arch also helps distribute the body’s weight evenly across the foot. An imbalance or weakness in this arch can cause or worsen plantar fasciitis. For example, flat feet, where the arch is almost nonexistent, or too high of an arch, can both increase the risk of this painful condition.
Plantar Fasciitis Symptoms and Signs
Primary symptoms of plantar fasciitis include sharp pain and sensitivity at the base of the heel. This pain might be more intense after a period of inactivity, like waking up in the morning, and may decrease after a few steps. Other symptoms can include arch pain and swelling. It’s also common to see patients with toe deformities showing similar symptoms, especially due to the affected metatarsophalangeal joint.
Several causes can contribute to plantar fasciitis. Foot biomechanics play a key role. Flat feet or a high foot arch can increase the risk. Other causes include:
- Wearing inappropriate shoes, too narrow or without adequate support.
- Being overweight, putting extra pressure on the feet.
- Intense physical activities or prolonged walking, especially among athletes.
- Certain conditions, like rheumatoid arthritis or Charcot-Marie-Tooth, can also be risk factors.
- Lastly, toe deformities, like hammer toe or claw toe, can also contribute to fasciitis.
The Impact of Daily Activities
Our modern lifestyle has evolved so that we spend more time standing, walking on hard surfaces, or engaging in intense sports. These activities exert continuous pressure on our feet, especially on the foot arch and heel. Activities like running on concrete, wearing unsuitable shoes for long hours, or merely standing for extended periods can provoke or exacerbate plantar fasciitis symptoms.
Comparison with Other Foot Conditions
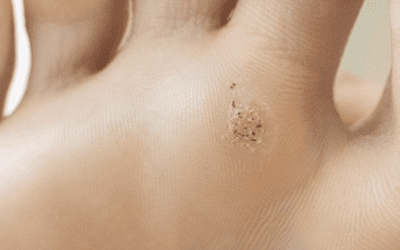
Plantar fasciitis is one of many conditions that can affect our feet. For instance, a bunion is a deformity of the big toe that can cause intense pain. Plantar warts are skin growths caused by a virus. But where plantar fasciitis stands out is its frequent association with repetitive activities or strains on the foot. Deformities like hammer toe or claw toe, which are abnormal toe positions, can also play a role in the onset of plantar fasciitis. These conditions alter how weight is distributed and exerted on the foot, leading to undue strain on the plantar fascia.
Prevention is key to avoiding plantar fasciitis. Recommendations include:
- Choosing shoes fitting the shape and function of your feet.
- Avoiding high heels and opting for good arch support.
- Incorporating strengthening and stretching exercises for feet and calves.
- Avoiding walking barefoot on hard surfaces.
- Regularly checking feet for deformities like bunions or corns.
The Importance of Shoes
Shoes are not just a fashion statement; they play a crucial role in our foot health. Unsuitable shoes, whether too narrow, lacking proper support, or with excessively high heels, can contribute to various issues, including plantar fasciitis. To prevent this condition, it’s essential to select shoes with good arch support, a flexible sole, and a spacious toe area. Shoe choice should match the intended activity. For example, someone who regularly walks or runs requires activity-specific shoes.
Prevention for Professionals
Professionals who spend many hours standing or frequently walk as part of their job, like nurses, teachers, or waitstaff, are particularly at risk of developing plantar fasciitis. The constant pressure on the fascia, combined with insufficient foot rest, can hasten the onset of symptoms. These professionals should be especially attentive to their shoe choices and consider orthotic inserts for added support. Regular breaks to stretch and rest the feet, coupled with mindfulness about posture and gait, can help prevent this painful condition.
Treatments Plantar Fasciitis
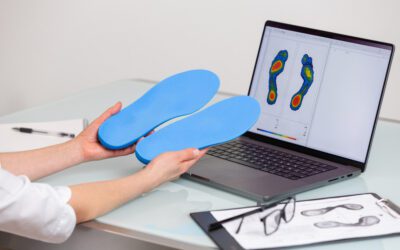
At-home treatment starts with rest, ice, compression, and elevation (the RICE protocol). Additionally, stretching exercises can help alleviate pain. Orthotic inserts can also be beneficial, especially when combined with other treatments. They support the foot arch and distribute pressure evenly.
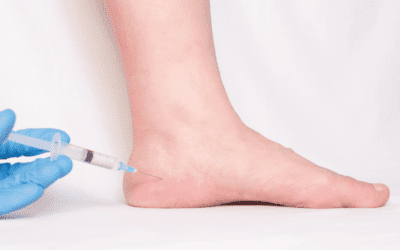
During a podiatrist consultation, a detailed evaluation determines the underlying cause. After examining the patient’s gait, the podiatrist may recommend custom-made orthotics or specific exercises.
Prevention Program
The professional environment often presents unique challenges for foot well-being. Here’s a program tailored for professionals, considering roles like nurses, teachers, and waitstaff:
- Shoe Selection: Versatility – Opt for shoes offering both comfort and support. Each profession might have specific needs (e.g., nurses might prefer non-slip shoes), but the core is a shoe that supports the arch and provides cushioning.
- Regular Breaks and Stretches: Micro-breaks – Plan short breaks to stretch your legs, especially if your job involves prolonged standing or sitting.
- Targeted Stretches: Incorporate simple stretches for feet, ankles, and calves into your daily routine. These can be done even during short breaks.
- Posture Management: Balancing – Professionals standing for long hours should be conscious of their posture to avoid excessive pressure on any part of their feet. Regularly shifting weight or using footrests can help.
- Weight Management: A balanced diet and physical activity tailored to your professional schedule will help maintain a healthy weight, reducing strain on the plantar fascia.
- Ergonomic Adjustments: Consider using anti-fatigue mats, especially for professions requiring long periods of standing in one spot.
- Continuing Education: Stay updated on new methods or products that can prevent foot pain. Workshops or seminars catering to specific professions on health and well-being at work might be available.